People often experience fungi in their kitchens, when breads or fruits rot turn mouldy. Fungi evolved 400 million years ago and they have various roles such as helping plants to move from their aquatic habitats to land to obtain minerals from the soil. Fungi also decompose organic litter and recycle the nutrients locked up in the leaves of the wood.
While fungal diseases are most commonly seen in plants but only a very small fraction of them assail humans. A few fungi, like Candida yeast, can sometimes kick off a serious infection but fungal infections rarely cause life-threatening complications in humans.
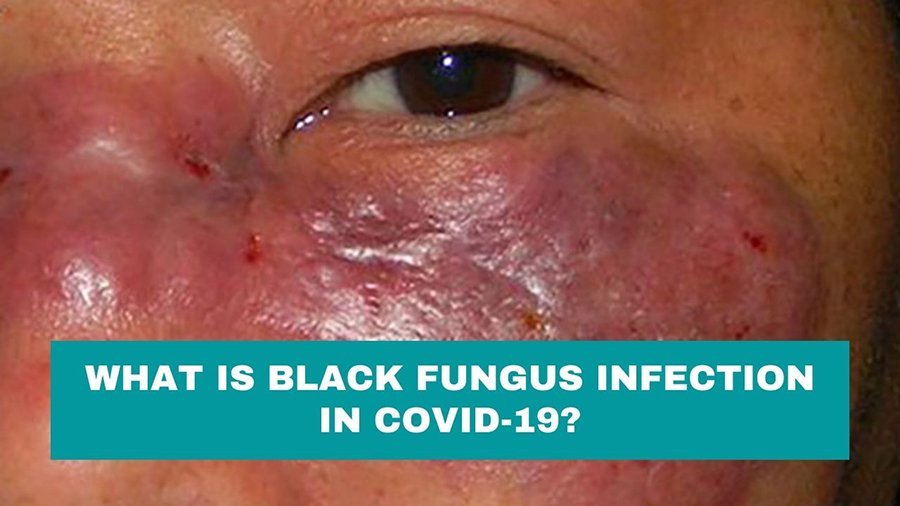
India is struggling due to the deadly surge of covid outbreak, doctors are now reporting cases of a rare infection called the “black fungus“, occurring among people recovering from the disease. It has been seen that there is a relation between COVID-19 and black fungus.
Like most fungi, Mucor produces millions of microscopic spherical, dark-hued structures called spores which are dispersed in air. When a patient whose immune system has been weakened due to infections, inhales the spores, he may develop mucormycosis. It can be debilitating or fatal if not treated quickly. Black fungus infection is quite rare and it is affecting people whose immune systems have been damaged by the coronavirus.
Patients suffering from COVID-19 have low immunity and are prone to developing mucormycosis. COVID-19 patients who have received steroids are particularly at a risk because steroids suppress the immune system. That’s why steroids should not be used unless absolutely necessary.
Many people who are recovering from COVID-19 have of late been afflicted by mucormycosis or black fungus. This fungus invades the sinus and makes the way to the intraorbital and intracranial regions. If its progression is not checked early, the patients could even die. It is normally not spread from person to person, but is found in the environment but due to the level of spread, it is too early to say how this is spreading.
In many experiments, it has been found that rats and rabbits who have inhaled the spores, these spores are quickly killed by white blood cells. But if the patient’s immune response has been suppressed, there is a production of less white blood cells by the body. In immune compromised conditions, the spores germinate and grow rapidly as thin and wire-like tubes that branch out and enter the blood vessels and kill them.
What are the Symptoms of Mucormycosis?
When black fungus attacks the sinuses, it spreads to the lungs, the brain and the central nervous system. Common symptoms when it affects lungs are:
- Fever
- Headache
- Facial pain
- Shortness of breath
- Swollen and reddish skin near the nose or eyes
When mucormycosis attacks the digestive system, the symptoms are:
- Abdominal pain
- Nausea
- Vomiting
- Gastrointestinal bleeding
How Black Fungus is Diagnosed?
Black fungus is diagnosed through a tissue biopsy and an X-ray of the lungs.
Who are at the Risk of Mucormycosis Infection?
People who have the following conditions are at the risk of developing mucormycosis:
- Uncontrolled diabetes
- Prolonged ICU / hospital stay
- Weakened immune system due to use of steroids
- Co-morbidities / post organ transplant / cancer
The healthy immune system successfully invades such fungal infections. COVID-19 affects the immune system. Moreover, the treatment of COVID-19 patients involves the intake of drugs like dexamethasone, which suppress the response of immune system. Due to these factors, COVID-19 patients face a higher risk of failing the battle against the attacks mounted by micro-organisms such as mucormycetes.
But this does not mean that every patient who suffer from coronavirus disease will get infected by mucormycosis. Black fungus in COVID-19 has been seen in diabetic patients. It can be fatal if not treated promptly. The chances of recovery depend upon early diagnosis as well as treatment.
There are a few simple steps that we can follow to lower the risk of contracting mucormycosis. These are:
- Patients should be aware of the disease.
- There should be periodically sampling of air in the hospitals, especially in the critically care wards.
- The humidifiers that are used during oxygen therapy must be sterile.
- Patients who are recovering should remain indoors until they regain their natural strength and immunity.