Abstract
Background: Oral Lichen Planus (OLP) is a chronic autoimmune inflammatory disorder affecting the oral mucosa, often accompanied by itching, burning sensations, and recurrent flares. Pediatric OLP is rare and commonly displays a prolonged course. From an Ayurvedic perspective, this condition correlates with Charmakushta, a Vata-Kapha dominant Kshudrakushta involving Twaka, Rakta, Mamsa, and Lasika. Chronicity, allergic symptoms, and mucosal damage suggest underlying Aam (toxin) accumulation, Dosha imbalance, and compromised local immunity.
Objectives: To evaluate the clinical improvements and therapeutic safety of an Ayurvedic intervention in a pediatric patient with Oral Lichen Planus (Charmakushta).
Materials & Methods: A 9-year-old female with a four-year history of oral mucosal lesions over the buccal mucosa and inner lips, along with recurrent skin rashes and allergic episodes, was managed exclusively using Ayurvedic treatment over multiple follow-ups between September 2022 and March 2024. The treatment protocol included internal administration of Swaras Chikitsa comprising Bhoomi Amla, Shirish, and later Changeri, along with IAFA Skin Detox Drops, Aahar Amrutham Chai, and classical Ayurvedic medicine Haridrakhandam. External therapy included IAFA E-5 Cell Repair Oil, IAFA 333 Shampoo, Yasthimadhu powder paste, Chaptex, and Hiora SG Gel. Dietary regulation, oral hygiene guidance, and anti-allergic lifestyle measures were also prescribed. Therapeutic response was evaluated through clinical examination of lesion resolution, reduction in dryness and irritation, and the frequency of allergic flare-ups reported during follow-up visits.
Results: Progressive and sustained improvement was observed, including marked reduction of mucosal lesions and dryness, controlled recurrence of allergic skin manifestations, and better overall oral comfort. Significant clinical relief was documented at each follow-up, especially by December 2023 and March 2024, with no adverse reactions reported throughout the treatment period.
Conclusion: Ayurvedic management demonstrated effective and safe remission of pediatric Oral Lichen Planus through immune modulation and mucosal tissue healing, indicating its potential as a reliable long-term therapeutic approach for OLP (Charmakushta) in children.
Introduction
Oral Lichen Planus (OLP) is a chronic, autoimmune-mediated inflammatory condition involving skin and mucous membranes. It is characterized clinically by persistent oral lesions, dryness, irritation, burning sensation, and periodic exacerbations that disturb normal daily functions such as eating and speaking.
In the oral cavity, it is commonly presented as white- gray lacy streaks, i.e., Wickham’s striae, erythematous patches, or painful erosions on the buccal mucosa and lips. Although OLP predominantly affects adults, pediatric involvement is increasingly recognized and is considered clinically challenging due to prolonged disease courses and hypersensitive mucosal response.
The chronic nature of OLP reflects an underlying dysregulation of immune function in which T-cell activation leads to basal epithelial damage and ongoing inflammation of the mucosa. Co-existing allergies, as seen in this case, further aggravate mucosal sensitivity and increase the chances of flare-ups. Modern treatment approaches rely mostly on topical corticosteroids and calcineurin inhibitors, etc.
While they may reduce inflammation temporarily, they carry long-term concerns in children, including local immunosuppression, mucosal atrophy, candida infections, and high relapse rates after discontinuation. Therefore, non-steroidal but effective management strategies are urgently needed in pediatric OLP. From the Ayurvedic perspective, this condition is closely correlated to Charmakushta, categorized under Kshudra Kushta due to its symptom pattern and chronic progression.
The disease is primarily Tridoshaja dominated by Vata-Kapha vitiation, affecting Twak, Rakta, Mamsa, and Lasika, leading to discoloration, roughness, thickening, persistent dryness, itching, and irritation. Additionally, long-standing allergic tendencies and inflammatory cycle suggest the presence of Aam (toxin) accumulation, impaired tissue metabolism (Dhatvagni dysfunction), and reduced mucosal defense (Ojas kshaya).
Hence, Ayurveda emphasizes a therapeutic plan that concentrates on Raktashodhana (blood purification to reduce inflammatory load), Aamapachana (correction of metabolic toxins), Vata-Kapha Shamana (restoring Doshic balance), Ojovardhana (immune regulation), and regeneration of the mucosal barrier (Twak-Mamsa Dhatu Poshana).
Internal herbal formulations help in systemic correction, while external soothing and reparative applications aim to restore epithelial structure and comfort. Dietary guidance, oral hygiene practices, and stress-free lifestyle modifications act as essential supportive measures in sustained healing.
This case report documents the successful Ayurvedic management of pediatric OLP with sustained remission, improved mucosal health, and absence of adverse effects, making it a valuable contribution toward the integration of Ayurveda in chronic oral autoimmune disorders.
Keywords: Oral Lichen Planus, Charmakushta, Ayurveda, Pediatric, Children, IAFA, Autoimmune Disease, Case Report, IAFA Skin Detox Drops
Case Presentation
A 9-year-old female presented with chronic oral lesions over the buccal mucosa and inner lips persisting for approximately four years, accompanied by recurrent skin rashes and allergic responses since childhood.
Symptoms had a fluctuating course with dryness, discomfort during exacerbations, and a history of frequent upper respiratory complaints earlier in life. Before Ayurvedic intervention, no mention of corticosteroid or immunosuppressive therapy was documented in the available clinical notes.
1) Patient Details
- Age/Sex – 9/F
- First Consultation – 19/09/2022
- Duration of symptoms – Approx 4 years
2) Chief Complaints
- White and reddish lesions inside the mouth, especially the buccal mucosa and under the lips
- Dryness and rash over the skin fold
- Itching and burning during flare-ups
- Recurrent allergic skin reactions since early childhood
3) Past Disease History
Repeated cough and cold at around 2.5 years of age
4) Family History
No family history of similar dermatological or autoimmune conditions was mentioned.
5) Diagnosis
Based on clinical features including chronicity, mucosal lesions, dryness, and itching, the patient was diagnosed with:-
Modern Diagnosis: Oral Lichen Planus
Ayurvedic Diagnosis: Charmakushta (Vata-Kapha predominant Kshudra Kushta)
Materials and Methods
1) Intervention Protocol
Treatment was initiated with Anta-Chikitsa (Internal therapy) to correct immune dysfunction and reduce inflammatory load. As the condition stabilized, topical mucosal repair therapies were introduced. Internal medicines were optimized over time to support tissue regeneration and maintain remission. Clinical tolerance and response were reviewed at every follow-up, and therapy was modified accordingly.
2) Ayurvedic Diagnostic Framework
Diagnosis was established as Vata-Kapha predominant Charmakushta based on chronic oral lesions, dryness, itching, discoloration, allergic triggers, and a history of recurrent respiratory issues.
Table 1. Ayurvedic Diagnostic Assessment
| Samprapti Ghataka | Findings |
| Vyadhi | Charmakushta |
| Dosha | Vata-Kapha dominant |
| Dushya | Twak, Rakta, Mamsa, Lasika |
| Strotas | Rasavaha, Raktavaha |
| Associated Vyadhi | Allergic skin reactions and URTI history |
3) Ayurvedic Treatment Protocol
Internal herbal formulations or Swarasa, like Bhoomi Amla, Shirish, and later Changeri, were administered orally for systemic immune modulation and Rakta Shodhana. IAFA Skin Detox formulations and Haridrakhandam were prescribed for Amapachana and inflammation control. External therapies such as E-5 Cell Repair Oil, 333 Shampoo, and later Yasthimadhu paste, Chaptex, and Hiora SG Gel were introduced to improve mucosal healing and prevent further irritation.
4) Treatment Progression Across Follow-Ups
Therapy was progressively escalated and modified throughout the follow-ups to match symptom shifts and healing status.
Table 2. Formulations used along with their dosage, frequency, route, time of administration, and duration
| Formulation | Dosage and Frequency | Route | Timing | Duration Status |
| Bhoomi Amla Swaras | 7.5 ml BID with equal water | Oral | 15-20 min after meals | Given continuously 19/09/2022 to 04/01/2023 → then paused during 05/04/2023 to 09/09/2023 (3 months gap) then again restarted from 11/12/2023 to 30/03/2024 |
| Shirish Swaras | 7.5 ml BID with equal water | Oral | 15-20 min after meals | Given continuously from 19/09/2022 to 04/01/2023 paused during 05/04/2023 to 09/09/2023 and again restarted from 11/12/2023 to 30/03/2024 |
| IAFA Skin Detox Drops | 2 ml BID in 20 ml water | Oral | After meals | Given 19/09/2022 to 04/01/2023, then stopped thereafter, replaced later with Skin Detox Tablets |
| Haridrakhandam | ½ tsp BID | Oral | After meals | Given continuously from 19/09/2022 to 04/01/2023 paused during 05/04/2023 to 09/09/2023 and again restarted from 11/12/2023 to 30/03/2024 |
| Aahar Amrutham Chai | 1 tsp BID | Oral | Morning and evening | Added on 04/01/2023. Stopped after 09/09/2023 follow-up. Not restarted |
| IAFA E-5 Cell Repair Oil | Topical twice daily | External | Morning and evening | Given continuously from 04/01/2023 to 30/03/2024 |
| IAFA 333 Shampoo | Apply and rinse | External | As directed | Given continuously from 04/01/2023 to 30/03/2024 |
| Changeri Swaras | 5 ml BID with equal water | Oral | Between meals | Added 30/03/2024 onward |
| IAFA Skin Detox Tablets | 1 tablet BID | Oral | After meals | Added 30/03/2024 onward |
| Yasthimadhu Choorna | Gargle and paste application | Oral/topical | Twice daily | Added 30/03/2024 onward |
| Chaptex | Thin coating on the lips | Topical | As advised | Added 30/03/2024 onward |
| Hiora SG Gel | Apply over oral lesions | Topical (buccal) | As advised | Added 30/03/2024 onward |
5) Phased Therapeutic Strategy
The Ayurvedic management in this case was given in a phased manner according to disease phase and clinical response. Each phase targeted a specific pathological layer, beginning from Dosha balancing and Ama reduction to structural mucosal repair and finally immune stabilization.
Table 3. Phased Ayurvedic Treatment Strategy
| Phase | Timeline | Key Ayurvedic treatment Active in Phase | Clinical Outcome Observed | Therapeutic Objective |
| Phase 1 – Dosha Shamana and Amapachana | 19/09/2022 to 04/01/2023 | Bhoomi Amla Swaras, Shirish Swaras, Skin Detox Drops, Haridrakhandam | Reduced oral irritation, a decrease in inflammatory symptoms, and a decrease in rash intensity | Balance Vata-Kapha and reduce toxin (Ama) load |
| Phase 2 – Mucosal Support and Barrier Repair | 04/01/2023 to 09/09/2023 | Haridrakhandam continued, IAFA E-5 Oil, IAFA 333 Shampoo, and Aahar Amrutham Chai added. | Improvement in dryness, barrier integrity maintained, symptomatic comfort | Strengthen Twak, Rakta, and results in epithelial healing |
| Phase 3 – Relapse Control Pause Window | 05/04/2023 to 09/09/2023 | Swaras temporarily paused | Minor symptom fluctuations but no severe flare-ups | Observation of disease stability and reducing the medicine load |
| Phase 4 – Regeneration and Immune Correction | 11/12/2023 to 30/03/2024 | Bhoomi Amla Swaras restarted, Shirish Swaras restarted, and Haridrakhandam restarted. Newly added Changeri Swaras, Skin Detox Tablets, Yasthimadhu Choorna | Visible lesion healing, dryness almost resolved, allergic episodes rare | Dhatu- Poshana, immune modulation, tissue rejuvenation |
| Phase 5 – Local Repair and Remission Maintenance | 30/03/2024 onward | Added Chaptex and Hiora SG Gel, E-5 Oil, and 333 Shampoo, continued | Oral mucosa stable, complete symptom control maintained | Long-term remission and relapse prevention |
6) Monitoring and Evaluation Protocol
Table 4. Clinical Monitoring Approach
| Parameter | Evaluation Frequency | Assessment Method | Response |
| Oral lesions | Every visit | Clinical visual examination | Marked regression |
| Lip dryness | Every visit | Patient and clinician scoring | Consistent improvement |
| Allergic flare-ups | Monthly review | Symptom history | Rare by the final stage |
| Burning or Pain | Each visit | Symptom inquiry | Minimal in the late phase |
| Treatment safety | Continuous | Observation for adverse effects | No adverse events |
7) Dietary and Lifestyle Monitoring
Lifestyle guidance included avoidance of irritating foods (spicy, acidic), maintaining regular sleep, and adopting cooling and soothing dietary options such as fennel, cumin, and green vegetables. Hydration with lukewarm water. Avoiding harsh oral products was strictly advised.
8) Ethical Considerations
This case involves a pediatric patient; therefore, ethical precautions were strictly followed throughout the course of treatment and documentation. Informed consent was obtained from the patient’s parent/guardian before the initiation of Ayurvedic therapy, with full explanation of the treatment plan, expected outcomes, and follow-up requirements.
Results
Table 4. Clinical Outcome Assessment Across Treatment Timeline
| Follow-up | Oral Lesions (Buccal Mucosa) | Lip Dryness | Skin Allergic Episodes | Burning / Irritation | Treatment Tolerance | Overall Clinical Status |
| Baseline (19/09/2022) | Persistent white/red lesions, visible inflammation | Severe | Frequent | Present | — | Symptomatic, chronic complaints |
| 04/01/2023 | Mild reduction in mucosal irritation | Moderate | Less frequent | Improved | Good | Initial response noted |
| 05/04/2023 | Stable condition maintained | Reduced intermittently | Occasional | Mild | Good | Progressive improvement |
| 05/07/2023 | Visible healing and less erythema | Mild | Rare episodes | Minimal | Good | Clear response, better oral comfort |
| 09/09/2023 | Continued improvement maintained | Mild | Rare | Minimal | Good | Condition stabilized |
| 11/12/2023 | Marked healing, lesions barely noticeable | Minimal dryness | No significant flare-ups | Negligible | Excellent | Significant clinical remission |
| 30/03/2024 | Near-complete resolution | Normal | Absent | None | Excellent | Sustained remission without relapse |
Table 5. Conclusion of the outcome Table
| Clinical Parameter | Baseline | Final Outcome (Mar 2024) | % Improvement |
| Mucosal Lesion Severity | High | Minimal or Healed | >75% |
| Dryness of Lips | High | Normal-Mild | Approx. 80% |
| Allergic Episodes | Frequent | Absent | 100% control |
| Pain/Burning | Noticeable | None | 100% relief |
| Safety/Tolerability | — | Excellent | — |
Discussion
Oral Lichen Planus (OLP) in children is a rare but chronic inflammatory condition driven by an inappropriate immune response against oral epithelial cells. Persistent relapse, mucosal sensitivity, dryness, and coexistence of allergic manifestations add complexity to its management. The present case achieved sustained remission through a structured and phased Ayurvedic approach.
1) Pathophysiological Understanding
OLP is an autoimmune T-cell–mediated disorder characterized by chronic lymphocytic infiltration at the basal membrane, degeneration of basal keratinocytes, oxidative stress, and altered epithelial healing and association with allergic conditions. Chronic immune activation results in repeated mucosal damage and thus poor epithelial turnover, which ends with persistent lesions.
From an Ayurvedic point of view, the disease aligns with Charmakushta, involving Vata-Kapha predominance and deeper tissue impairment. The Dushya involvement included Twak, Rakta, Mamsa, and Lasika, indicating disrupted tissue nutrition, immune imbalance, and chronicity. Ama accumulation and Rasavaha-Raktavaha Strotas dysfunction further contributed to recurrent flare-ups, while Ojas Kshaya explained reduced mucosal function.
A phased therapeutic approach was followed to correct the pathology stage-wise. Initial treatment focused on Dosha- Shamana and Amapachana using Various Swaras orally along with detoxifying formulations, which reduced mucosal irritation and allergic frequency. Subsequent topical therapies strengthened Twak and Rakta and prevented surface irritation, resulting in improvement in dryness and lesion appearance.
Restarting Swaras along with mucosal regenerative agents promoted Mamsa dhatu repair and epithelial healing. Lasika dusti and immune hypersensitivity were addressed in later phases through immune-supportive medicines and barrier-stabilizing applications, leading to sustained remission.
2) Phase-Wise Therapeutic Protocol
Phase-1: Dosha-Shamana and Ama-Pachana Phase i.e., 19/09/2022 to 04/01/2023
Initially, the treatment plan focused on correcting the aggravated Vata-Kapha and reducing Ama formation to control the inflammatory and allergic tendencies. Internal medications, including Bhoomi Amla Swaras, Shirish Swaras, IAFA Skin Detox Drops, and Haridrakhandam, were administered to purify Rakta and restore mucosal balance. During this period, oral irritation, inflammatory response, and allergic flare episodes gradually reduced, indicating early stabilization of the disease pathology.
Phase-2: Mucosal Barrier Support and Symptom Relief, i.e., 04/01/2023 to 09/09/2023
With improvement in inflammatory signs, therapy progressed toward enhancing epithelial integrity and reducing dryness. External applications such as IAFA E-5 Cell Repair Oil and IAFA 333 Shampoo were introduced along with supportive internal formulation Aahar Amrutham Chai. This phase improved the lubrication and nourishment of the oral mucosa and skin, resulting in a noticeable decline in dryness, lesion thickness, and local discomfort.
Phase-3: Dhatu-Poshana and Epithelial Regeneration, i.e., 11/12/2023 to 30/03/2024
After partial remission, regenerative therapy was initiated to strengthen Mamsa Dhatu and correct deeper Dushya involvement, especially of Twak, Rakta, and Lasika. Bhoomi Amla Swaras and Shirish Swaras were restarted along with Changeri Swaras and IAFA Skin Detox Tablets for immunological and structural rejuvenation. Yasthimadhu Choorna was added for local healing. During this phase, oral lesions showed marked resolution with near-normal mucosal texture.
Phase-4: Immune Stabilization and Remission Maintenance Phase, i.e., 30/03/2024 onward
The final phase emphasized long-term mucosal protection and prevention of relapses. Local protective agents such as Chaptex and Hiora SG Gel were incorporated to maintain hydration, barrier function, and symptom-free status. This supported Lasika and Ojas’ stability, resulting in sustained remission without recurrence of lesions or allergic episodes.
3) Pharmacological Correlation
Table 5. Ayurvedic Medicines and Their Pharmacological Correlation
| Formulation | Classical Actions | Major Active Phytochemicals | Modern Pharmacological Correlation |
| Bhoomi Amla (Phyllanthus niruri) | Raktashodhaka, Pitta-Kapha-Shamana | Phyllanthin, Hypophyllanthi, Corilagin | Anti-inflammatory, antioxidant, hepatoprotective, supports mucosal healing and immune regulation. |
| Shirish (Albizia lebbeck) | Ojovardhana, Kapha-Vata Hara, Sothahara | Triterpenoids, Saponins, Flavonoids | Anti-allergic, mast-cell stabilization, reduces histamine-mediated mucosal irritation. |
| Changeri (Oxalis corniculata) | Tridosha-Shamana, Deepana-Pachana | Vitamin C, Phenolic antioxidants | Improves tissue metabolism, epithelial repair, and free-radical scavenging |
| Haridrakhandam | Amapachana, Kapha-Vatahara, Raktaprasadana | Curcumin, Piperine | Immunomodulatory, anti-inflammatory, supports epithelial regeneration |
| Skin Detox Drops/Tablets | Raktashodhaka, Vata-Kapha shamana | Alkaloids, Tannins, Flavonoids | Reduces inflammatory cytokines, detoxification, and improves microcirculation |
| Yasthimadhu (Glycyrrhiza glabra) | Vranaropana, Pitta-Vatshara, Prashamana | Glycyrrhizin, Liquiritigenin | Mucosal protection, accelerating epithelialization, and analgesic activity |
| E-5 Cell Repair Oil | Twak- Poshana, Vata-Kaphahara | Fatty acids and herbal actives | Skin barrier restoration, irritation reduction, and moisture retention |
| Chaptex (lip barrier protector) | Snehana, Sothahara | Bioadhesive lipids | Prevents dryness-induced epithelial cracking |
| Hiora SG Gel (oral protective gel) | Local healing support | Bio-adhesive polymers, plant extracts | Forms protective film, promotes mucosal recovery |
e symptoms has been observed. 90% of her disease on diction got cured completely and later on Dr Gupta advised to get online follow-ups for another 3 months as the medications involved not only eliminating the diseases but also boosting the immunity.
Complete Recovery
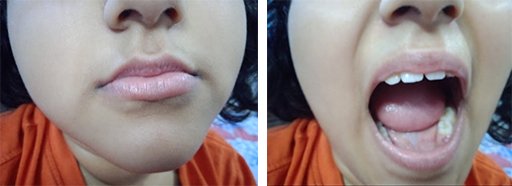
Previously all the ridges of her tongue and the roof of her mouth were filled with white patches, added to that, the swelling and itching of her outer lips. All recovered after getting safe and effective treatment from IAFA Ayurveda.
Happy Note
Source:- https://g.co/kgs/L4mGv2
Conclusion
This case of Oral Lichen Planus showed steady and consistent improvement with a phased Ayurvedic treatment approach. The therapy helped reduce inflammation, dryness, and allergic tendencies while promoting healthy healing of the oral lining.

Clinical progress was maintained without relapse, and no steroids were required at any stage. Overall, the outcome highlights that Ayurveda can serve as a safe and effective option for long-term management of Oral Lichen Planus in younger individuals, with noticeable improvement in oral comfort and daily functioning.
References
- Lavanya N, Jayanthi P, Rao UK, Ranganathan K. Oral lichen planus: An update on pathogenesis and treatment. J Oral Maxillofac Pathol. 2011 May; 15 (2): 127- 32. doi: 10. 4103/ 0973- 029X. 84474. PMID: 22529568; PMCID: PMC- 3329692.
- Kumawat, Priyanka & Unadkat, Rajshree. (2024). Ayurveda management of Oral Lichen Planus. Journal of Ayurveda and Integrated Medical Sciences. 9. 262- 267. 10. 21760/ jaims. 9. 8. 40.
- https://www.mayoclinic.org/diseases-conditions/oral-lichen-planus/symptoms-causes
- Mohan Das U, JP B. Oral lichen planus in children. Int J Clin Pediatr Dent. 2009 Jan; 2 (1): 49- 51. doi: 10. 5005/ jp- journals- 10005- 1043. Epub 2009 Apr 26. PMID: 2520- 6101; PMCID: PMC- 4086552.
- Jadhav, Dr & Paliwal, Amit & Babar, Dr & Jadhav, Dr & Patil, Priyanka. (2025). Holistic Approaches to Oral Lichen Planus: Insights from Ayurvedic Treatment. Journal of Emerging Technologies and Innovative Research. 12. 10. 56975/ jetir. v12i4. 560809.
- Bilapate, Dr. (2025). Ayurvedic Management of Oral Lichen Planus (Charma Kushta): A Case-Based Approach. 398- 403. 10. 37648/ medinity-2025. 062.
- Ratha, Kshirod & Barik, Laxmidhar & Panda, Ashok & Hazra, Jayram. (2016). A single case study of treating hypertrophic lichen planus with Ayurvedic medicine. AYU (An international quarterly journal of research in Ayurveda). 37. 56. 10. 4103/ ayu. AYU- 1- 16.
- Nampalliwar, Amit & Biradar, Dr. (2021). AYURVEDIC MANAGEMENT OF LICHEN PLANUS: A CASE REPORT. International Ayurvedic Medical Journal. p5. 3043- 3049. 10. 46607/ iamjp- 145052021.
- Chinnasamy NK, Venugopal DC, Sankarapandian S, Narasimhan M. Oral Lichen Planus in a 7-year-old Child: A Rare Case Report. Int J Clin Pediatr Dent. 2020 Jan- Feb; 13 (1): 91- 93. doi: 10. 5005/ jp- journals- 10005-1713. PMID: 32581487; PMCID: PMC- 7299881.
- Gupta S, Jawanda MK. Oral Lichen Planus: An Update on Etiology, Pathogenesis, Clinical Presentation, Diagnosis, and Management. Indian J Dermatol. May- Jun; 60 (3): 222- 9. doi: 10. 4103/ 0019- 5154. 156315. PMID: 26120146; PMCID: PMC- 4458931.
- Gururaj N, Hasinidevi P, Janani V, Divynadaniel T. Diagnosis and management of oral lichen planus – Review. J Oral Maxillofac Pathol. 2021 Sep- Dec; 25 (3): 383- 393. doi: 10. 4103/ jomfp. Jomfp- 386- 21. Epub 2022 Jan 11. PMID: 3528- 1147; PMCID: PMC- 8859620.
- Andabak- Rogulj A, Vindis E, Aleksijevic LH, Skrinjar I, Juras DV, Ascic A, Brzak BL. Different Treatment Modalities of Oral Lichen Planus: Narrative Review. Dent J (Basel). 2023 Jan 12; 11 (1): 26. doi: 10. 3390/ dj- 11010026. PMID: 36661563; PMCID: PMC- 9857452.
- Singh V, Pal M, Gupta S, Tiwari SK, Malkunje L, Das S. Turmeric – A new treatment option for lichen planus: A pilot study. Natl J Maxillofac Surg. 2013 Jul; 4 (2): 198- 201. Doi: 10. 4103/ 0975- 5950. 127651. PMID: 24665176; PMCID: PMC- 3961895.
- Ratha, K. K., Barik, L., Panda, A. K., & Hazra, J. (2016). A single case study of treating hypertrophic lichen planus with Ayurvedic medicine. Ayu, 37 (1), 56. https:// doi. org/ 10. 4103/. AYU_1_16
- Kalaskar AR, Bhowate RR, Kalaskar RR, Walde SR, Ramteke RD, Banode PP. Efficacy of Herbal Interventions in Oral Lichen Planus: A Systematic Review. Contemp Clin Dent. 2020 Oct- Dec; 11 (4): 311- 319. doi: 10. 4103/ ccd. ccd_320_20. Epub 2020 Dec 20. PMID: 3385- 0395; PMCID: PMC- 8035840.
- Louisy A, Humbert E, Samimi M. Oral Lichen Planus: An Update on Diagnosis and Management. A.m J Clin Dermatol. 2024 Jan; 25 (1): 35- 53. doi: 10. 1007/ s40257- 023- 00814- 3. Epub 2023 Sep 15. PMID: 3771-3153.
- Nanda A, Al-Ajmi HS, Al-Sabah H, et al. Childhood lichen planus: A report of 23 cases. Pediatr Dermatol. 2001; 18 (1): 1– 4. doi: 10. 1046/ j. 1525-1470. 2001. 018001001. x.
- Chatterjee K, Bhattacharya S, Mukherjee CG, Mazumdar A. A retrospective study of oral lichen planus in the paediatric population. J Oral Maxillofac Pathol. 2012 Sep; 16 (3): 363- 7. doi: 10. 4103/ 0973- 029X. 102486. PMID: 23248468; PMCID: PMC- 3519211.
- Thapa DM, Malathi M. Management of childhood lichen planus. Nepal Journal of Dermatology, Venereology & Leprology. 2016; 12 (1): 1– 6. doi: 10. 3126/ njdvl. v12i1. 10588.
- Spirito F, Dioguardi M, Caponio VC, Ambrosino M, Lo Muzio E, Lo Muzio L. Oral lichen planus in children: A systematic review. Med Oral Patol Oral Cir Bucal. 2024 Mar 1; 29 (2): e152- e162. Doi: 10. 4317/ medoral. 25938. PMID: 38288854; PMCID: PMC- 10945876.
- Sharma G, Sardana D, Vohra P, Rehani S, Nagpal A. Oral Lichen Planus in a Pediatric Patient: A Novel Therapeutic Approach. J Dent (Tehran). 2017 Mar; 14 (2): 109- 114. PMID: 29104603; PMCID: PMC- 5662509.
- Spirito F, Caponio VCA, Lo Muzio E, Campisi G, Santarelli A, Lo Russo L, Rubini C, Favia G, Limongelli L, Coppola N, Lo Muzio L, Leuci S. Oral lichen planus in children: An Italian case series. Pediatr Dermatol. 2023 May- Jun; 40 (3): 489- 493. doi: 10. 1111/ pde. 15318. Epub 2023 Apr 5. PMID: 3701- 9629.
- Hasan S, Mansoori S, Ansari MI, Siddiqui S. Oral lichen planus in an 8-year-old child: A case report with a brief literature review. J Oral Maxillofac Pathol. 2020 Feb; 24 (Suppl 1): S128- S134. Doi: 10. 4103/ jomfp. JOMFP- 343- 19. Epub 2020 Feb 28. PMID: 32189921; PMCID: PMC- 7069139.








